Sickle cell anemia
(Sickle Cell Disease)
Sickle cell anemia – Definition
Sickle cell anemia is a genetic disorder. It alters the shape of the red blood cells (RBCs). This decreases their ability to carry oxygen. It can also cause acute episodes of pain. These are called a sickle cell crisis. The body will also destroy the sickle cells. The loss of RBCs results in anemia.
The change in the ability and number of RBCs can decrease the amount of oxygen for the body.
Sickle cell anemia – Causes
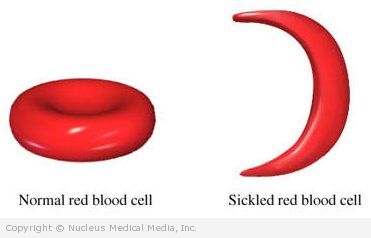
RBCs are normally soft and round. This helps them move easily through the blood vessels. A main building block of the RBC is hemoglobin.
People with sickle cell anemia have an abnormal type of hemoglobin. It causes the red blood cells to become hard and sickle-shaped. Because of their odd shape, some of the cells get stuck in the small blood vessels. There they break apart. The broken parts can cause blockages in the vessels. This can happen in a blood vessel that leads to a major organ. The decreased blood flow can cause severe pain and organ damage.
The body also recognizes that sickled cells are abnormal. The body will destroy them faster than they can be replaced. This causes anemia especially under the following conditions:
- Fever
- Infection
- Dehydration
- Drop in oxygen or change in air pressure (sometimes occurs during airplane travel)
Sickle cell anemia – Risk Factors
Factors that increase your chance for sickle cell anemia include:
- Genetics: the defective gene needs to be inherited from both parents to have the disease
- Race: Blacks of sub-Saharan origin
- Ethnicity: Greeks, Italians, and people from some parts of India, Central and South America, and the Arabian Peninsula
Sickle cell anemia – Symptoms
This condition produces a group of symptoms known as a sickle cell crisis. These are episodes of pain that occur with varying frequency and severity. It is usually followed by periods of remission. The risk for a sickle cell crisis increases with any activity that boosts the body’s requirement for oxygen. This may include illness, physical stress, or high altitudes.
These painful crises can last hours to days. They affect the bones of the back, the long bones, and the chest. The crises can be severe enough to require hospital admission for pain control and IV fluids.
Symptoms of impending sickle cell crisis include:
- Pain and swelling in the hands and feet
- Fever
- Jaundice
- Anemia
- Chest pain, or episodic pain in joints, abdomen, or back
- Shortness of breath
- Fatigue
- Abdominal swelling
- Unusual or prolonged headache
- Any sudden weakness or loss of sensation
- Priapism (prolonged erection)
- Sudden vision changes
- Sudden, severe anemia can cause:
- Weakness
- Shortness of breath
- Heart failure
- Shock
- Loss of consciousness
Complications of sickle cell anemia include:
- Destruction of the spleen
- Severe bacterial infections:
- Pneumonia
- Meningitis
- Kidney and bone infections
- Damage to the joints (especially hip and shoulder)
- Gallstones
- Damage to eyes, resulting in impaired vision
- Stroke or other neurological impairment
- Seizures
- Liver disease
- High rate of hepatitis C
- Damage to penis, due to priapism (may result in impotence)
- Leg ulcers
- Heart murmurs or enlarged heart
- Delayed growth
- Delayed sexual development
- Problems with thinking, memory, and performance
Sickle cell anemia – Diagnosis
Hemoglobin electrophoresis is a simple blood test. It can be done by a doctor or local sickle cell foundation. Most states require testing of newborns for sickle cell.
Amniocentesis is a form of prenatal testing. It can also detect sickle cell disease.
Sickle cell anemia – Treatment
Basic treatment of sickle cell crisis includes:
- Bed rest
- Pain relief medicines
- Oral and intravenous fluids
- Oxygen — to reduce pain and prevent complications
In addition, treatment may include:
Penicillin
Newborns with sickle cell disease may be given penicillin. It is given twice a day, beginning at age two months. It is continued until at least five years of age.
Pneumococcal Vaccine
It is recommended that children with sickle cell disease who are 2-5 years of age receive pneumococcal vaccine (PCV-7).
Hydroxyurea (Hydrea)
Hydroxyurea (Hydrea) is the first drug to significantly prevent complications of sickle cell disease. It increases the production of fetal hemoglobin. This decreases the number of deformed red blood cells. As a result, it reduces the frequency of sickle cell crisis. Hydrea is not appropriate for everyone with sickle cell disease. It is only recommended for people over age 18 who have had at least three painful crises in the previous year.
Blood Transfusions
Blood transfusions can treat and prevent some of the complications. Transfusion therapy can help prevent recurring strokes in children.
Bone Marrow Transplant
A bone marrow transplant from a matched donor may be effective. There are medical risks involved. Recipients must also take drugs that suppress the immune system for the rest of their lives.
If you or your child is diagnosed with sickle cell anemia, follow your doctor’s instructions.
Sickle cell anemia – Prevention
Sickle cell anemia cannot be prevented. There are some general guidelines that may keep the condition under control. Be sure to discuss these with your doctor:
- Take daily folic acid supplements. This will help to build new red blood cells.
- Drink plenty of water to prevent dehydration.
- Avoid temperature extremes.
- Avoid overexertion and stress.
- Get plenty of rest.
- Get regular check-ups with knowledgeable healthcare providers.
- Seek genetic counseling.