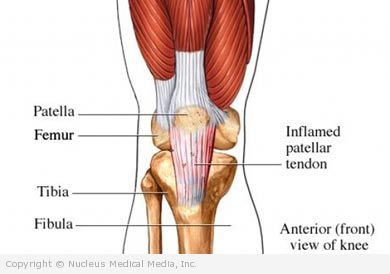
Patellar tendinopathy
(Jumper’s Knee; Patellar Tendonitis; Patellar Tendinosis; Quadriceps Tendonitis; Infrapatellar Tendinopathy; Patellar Apicitis)
Patellar tendinopathy – Definition
Tendinopathy is an injury to the tendon. It can cause pain, swelling, and limit movement. The injuries can include:
- Tendonitis — an inflammation of the tendon (Although this term is used often, most cases of tendinopathy are not associated with significant inflammation.)
- Tendinosis — microtears (tiny breaks) in the tendon tissue with no significant inflammation
The patellar tendon connects the patella (kneecap) to the lower leg bone (tibia). Tendinopathy and the associated pain may take months to resolve.
Patellar tendinopathy – Causes
Tendinopathy is generally caused by overuse of a muscle-tendon unit. Over time, the strain on the tendon causes structural changes within the tendon itself.
Patellar tendinopathy occurs from overuse of the knee tendon. Overuse may be caused by any activity that requires:
- Intense running
- Jumping
- Frequent stops and starts
- Frequent impact to the knee
Patellar tendinopathy is most common in the following sports:
- Basketball
- Soccer
- Volleyball
- Running
Patellar tendinopathy – Risk Factors
Factors that increase your chance of patellar tendonopathy include:
- An increase in the frequency of training
- A sudden increase in the intensity of training
- Changing from one sport to another
- Training on a hard surface
- Repeated improper movements while training
- Muscle weakness or imbalance
Patellar tendinopathy – Symptoms
Symptoms include:
- Pain and tenderness in the patellar tendon below the knee
- Pain or tightness in the knee when bending, squatting, or straightening the leg
- Discomfort in the knee when jumping, running, or walking
Patellar tendinopathy – Diagnosis
The doctor will ask about your symptoms, physical activity, and how the injury occurred. The doctor will also examine your knee, and may ask you to perform certain movements.
In some cases your doctor may order:
- X-ray — a test that uses radiation to take a picture of structures inside the body, used to rule out other conditions that may be causing your symptoms
- MRI scan — a test that uses magnetic waves to make pictures of structures inside the body, used to check the severity of your condition
Patellar tendinopathy – Treatment
Treatment includes:
Ice and Rest
Apply ice or a cold pack to the knee for 15-20 minutes, every four hours, for 2-3 days. Wrap the ice or cold pack in a towel. Do not apply the ice directly to your skin.
Avoid the activity that caused the pain. Reduce shock or vibrations to the knee.
Medication
Over-the-counter medicines that are commonly used to reduce pain include:
- Ibuprofen (Motrin, Advil)
- Naproxen (Aleve, Naprosyn)
- Acetaminophen (Tylenol)
- Aspirin
Topical pain medicines (eg, creams, patches) applied to the skin are another option.
Infra-patellar Strap
This strap (also called a counterforce brace) can help support the tendon and reduce pain. It is worn as a band just below the knee.
Physical Therapy
Physical therapy will help:
- Stretch and condition the quadriceps muscle, which attaches to the patella
- Maintain muscle strength, flexibility, and endurance
Cortisone Injections
If the treatments above do not reduce inflammation, some doctors may recommend that you consider a cortisone injection. Check with your doctor to find out what is best for you. Avoid repeated cortisone injections.
Resuming Exercise
Return to high-impact physical activity gradually. Healing has occurred when:
- The knee can bend and straighten without pain.
- You are able to jump on the injured leg without pain.
- You are able to jog in a straight line without pain.
- Swelling is gone.
- Normal strength of the quadriceps muscles has returned.
Surgery
You may need surgery if there is:
- Advanced damage to the tendon
- Little or no response to other treatments over a 6-12 month period
Patellar tendinopathy – Prevention
You may prevent patellar tendinopathy by:
- Avoiding activities and sports that repeatedly stress the kneecaps
- Gradually increasing the frequency and intensity of exercise
- Regularly doing quadriceps muscle stretching and strengthening exercises