(Degenerative Joint Disease; Arthritis, Osteo-)
Osteoarthritis – Definition
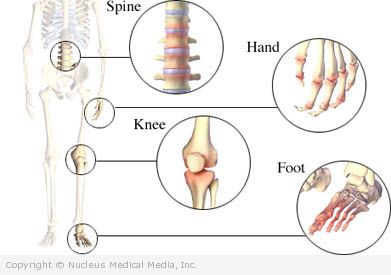
Osteoarthritis is the breakdown of cartilage in the joints. This is followed by chronic inflammation of the joint lining. Healthy cartilage is a cushion between the bones in a joint. Osteoarthritis usually affects the hands, feet, spine, hips, and knees. People with osteoarthritis usually have joint pain and limited movement of the affected joint.
Osteoarthritis – Causes
The exact cause is unclear.
Osteoarthritis – Risk Factors
Risk factors include:
- Being overweight or obese
- Having a family history of osteoarthritis
- Having an injury to the joint surface
- Having an occupation or doing physical activities that put stress on joints
- Having an endocrine disorder (eg, diabetes)
- Being older
Osteoarthritis – Symptoms
Symptoms include:
- Mild to severe pain in a joint, especially after overuse or long periods of inactivity, such as sitting for a long time
- Creaking or grating sound in the joint
- Swelling, stiffness, limited movement of the joint, especially in the morning
- Weakness in muscles around the sore joint
- Deformity of the joint
Other symptoms include loss of cartilage, bone spurs around the joint, and muscle weakness of the extremity.
Osteoarthritis – Diagnosis
The doctor will ask about your symptoms and medical history, and perform a physical exam.
Tests may include:
- X-ray — a test that uses radiation to take a picture of structures inside the body, especially bones
- Blood tests
- Arthrocentesis — a procedure that involves withdrawing fluid from a joint
Osteoarthritis – Treatment
There is no treatment that stops cartilage loss or repairs cartilage that is damaged. The goal of treatment is to reduce joint pain and inflammation and to improve joint function.
Treatments may include:
Medications
- Over-the-counter pain medicine
- Acetaminophen (eg, Tylenol) and nonsteroidal anti-inflammatory drugs (NSAIDs), such as ibuprofen (eg, Advil) and naproxen (eg, Aleve)
- Topical pain medicines (eg, creams, patches) that are applied to the skin, such as capsaicin, methyl salicylate, menthol, diclofenac
- Prescription pain medicine, such as:
- Diclofenac and misoprostol (Arthrotec) — nonsteroidal anti-inflammatory drug; may reduce the risk for gastrointestinal bleeding
- Opiates and opiate-like medicines
- Antidepressants, such as duloxetine (Cymbalta) — may be prescribed to treat chronic pain from osteoarthritis
- Viscosupplementation — injection of a substance called hyaluronan into the joint, which helps lubricate the joint
Dietary Supplements
Glucosamine and chondroitin are two commonly used supplements. But, research has shown that these supplements are not beneficial for most people with osteoarthritis. Talk with your doctor before taking any herbs or supplements.
Alternative Treatments
Some doctors report that acupuncture has been successful in reducing the pain of osteoarthritis, although the evidence is not consistent.
While more studies are needed, balneotherapy (hot water therapy), relaxation therapy, exercise, yoga, and tai chi may be helpful.
Mechanical Aids
Shoes with shock-absorbing soles may provide some relief while you are doing daily activities or exercising. Splints or braces help to properly align joints and distribute weight. Knee and wrist joints may benefit from elastic supports. A neck brace or corset may relieve back pain. Also, a firm mattress may help chronic back pain. Canes, crutches, walkers, and orthopedic shoes also can help those with advanced osteoarthritis in the lower body.
Weight Reduction
Losing weight can lessen the stress on joints affected by osteoarthritis. Losing five pounds can eliminate at least 15 pounds of stressful impact for each step taken. The more weight lost, the greater the benefit.
Exercise and Physical Therapy
Strengthening the muscles supporting an arthritic joint (particularly the knee, lower back, and neck) may decrease pain and absorb energy around the joint. For example, if you have arthritis in the knee, exercise, including strength training, can also help improve knee function.
Swimming and water aerobics are good options because they do not put stress on the joint.
Another option is transcutaneous electrical nerve stimulation (TENS). With TENS, you are connected to a machine that sends electrical signals through the skin to nerves. This type of therapy may decrease pain in some people.
Assistive Devices
If you are having difficulty getting around due to arthritis pain, your doctor might recommend that you install handrails and grips throughout your home. These are useful in the bathroom and shower. You may need elevated seats (including toilet seats) if you’re having difficulty rising after sitting.
Heat and Ice
Applying heat (with hot water bottles or heating pads) helps joints and muscles move more easily. It can also lessen pain. Using ice packs after activity can also help.
Manual Therapy
If you have knee osteoarthritis, manual therapy (including massage therapy and manipulation) may be helpful.
Steroids
Corticosteroid injections to the inflamed joint may be given if other pain medicines do not work. Because repeated cortisone injections can be harmful to the cartilage, they are reserved for those with severe symptoms.
Surgery
Surgery can:
- Reposition bones to redistribute stress on the joint
- Replace joints
- Remove loose pieces of bone or cartilage from joints
Osteoarthritis – Prevention
To reduce your chance of getting osteoarthritis:
- Maintain a healthy weight.
- Do regular, gentle exercise (eg, walking, stretching, swimming, yoga).
- Avoid repetitive motions and risky activities that may contribute to joint injury, especially after age 40.
- With advancing age, certain activities may have to be dropped or modified. But, continue to be active.