Muscular Dystrophy – MD
Muscular Dystrophy – Definition
Muscular dystrophy is a group of inherited, progressive muscle disorders. All forms cause progressive weakness and degeneration of the muscles that control movement. Some also affect the heart or other organs. Age of onset is between infancy to adulthood. The different forms include:
- Duchenne dystrophy (the most common)
- Becker (a milder form than Duchenne)
- Myotonic muscular dystrophy (can have its onset in late adulthood)
Muscular Dystrophy – Causes
This condition is caused by defects in genes that control muscle development and function. In some cases, the genes are passed from parent to child. In other cases, the genetic mutation occurs spontaneously.
Muscular Dystrophy – Risk Factors
These factors increase your chance of developing muscular dystrophy. Tell your doctor if you have any of these risk factors:
- Family member with muscular dystrophy
- Sex: male for some types (Duchenne and Becker)
Muscular Dystrophy – Symptoms
Symptoms common to most forms of muscular dystrophy may include:
Initial symptoms:
- Progressive weakening of muscles—Usually, those muscles closest to the trunk become weak first. Then, muscles further away weaken as the disease advances.
- Enlargement of muscles as they weaken
- Clumsiness
- Frequent falling and difficulty getting up
Later symptoms:
- Severe muscle deterioration, usually leading to use of a wheelchair
- Distortion of the body
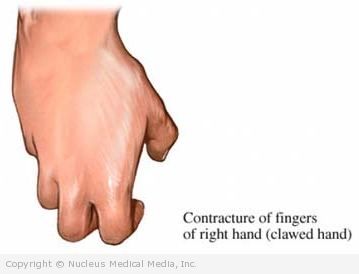
- Muscle contraction and stiffening (often severe)
- Difficulty breathing
Symptoms specific to Duchenne and Becker dystrophy include:
- Abnormally curved spine
- Enlargement and weakening of the heart muscle
- Pneumonia and other respiratory infections
Symptoms specific to myotonic muscular dystrophy include:
- Difficulty in letting go after a handshake
- Muscle weakness that affects the central nervous system, heart, digestive tract, glands, or eyes
- Symptoms usually become progressively worse. In many forms, life expectancy is shortened.
Muscular Dystrophy – Diagnosis
The doctor will ask about your symptoms and medical history. She will also do a physical exam.
Tests may include:
- Muscle tissue biopsy — removal of a sample of muscle tissue for testing
- Blood enzyme tests — testing a blood sample to look for elevated enzyme levels
- Genetic testing-using blood samples
- Electromyogram (EMG) — measures electrical impulses coming from muscles
- Nerve conduction study (NCS) — measures electrical impulses in the nerves
Muscular Dystrophy – Treatment
There is no cure. However, treatment may help improve the symptoms.
Treatment may consist of:
Physical Therapy and Exercise
Physical therapy and exercise can help prevent the muscles from permanently contracting and stiffening.
Braces
In earlier stages, wearing braces may improve your ability to move around. A back brace may slow curvature of the spine.
Medication
Medicines may include:
- Corticosteroids to relieve muscle weakness (chronic steroids can also cause muscle injury called “steroid myopathy”)
- Creatine supplements (shown to reduce fatigue and increase strength in some studies)
- Drugs for heart problems if muscular dystrophy affects the heart
Much research is being done in this area. A new technique called “gene transfer” therapy has been used with some good early results in certain forms of dystrophy.
Surgery
In severe cases, surgery may be needed to release muscles that are painfully tight. If there are heart problems, a pacemaker may be needed.
Muscular Dystrophy – Prevention
Muscular dystrophy is an inherited disease. Get genetic counseling if you are concerned about having a child with muscular dystrophy, especially if you:
- Have muscular dystrophy or a family history of the disease
- May be a carrier of the gene for muscular dystrophy
- Have a partner with a family history of the disease