Atrial fibrillation
Atrial fibrillation – Definition
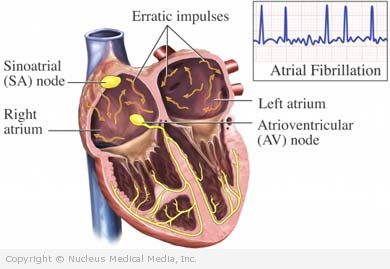
Atrial fibrillation is an abnormal heart rhythm. The heart’s electrical system normally sends regularly spaced, predictable signals, telling the heart muscle to contract, or beat.
The heart has two upper chambers, called atria, and two lower chambers, called ventricles. Each signal starts in the atria and travels to the rest of the heart. In atrial fibrillation, the electrical signals from the atria are fast and irregular. The atria quiver, rather than contract. Some signals do not reach the ventricles and the ventricles continue pumping, usually irregularly and sometimes rapidly. This uncoordinated rhythm can reduce the heart’s efficiency at pumping blood out to the body. Blood left in the heart chambers can form clots. These clots may sometimes break away, travel to the brain, and cause a stroke.
Atrial fibrillation – Causes
In most cases, atrial fibrillation is due to an existing heart condition. But atrial fibrillation can occur in people with no structural heart problems. A thyroid disorder or other condition may cause the abnormal rhythm. In some cases, the cause is unknown.
Atrial fibrillation – Risk Factors
Factors that may increase the risk of atrial fibrillation include:
- Age: 55 or older
- Sex: male
- Family history of atrial fibrillation
- Cardiovascular diseases, such as high blood pressure, coronary artery disease, congestive heart failure, heart attack, heart valve disease, endocarditis, cardiomyopathy, congenital heart disease, prior episode of atrial fibrillation
- Lung diseases, such as emphysema, asthma, blood clots in the lungs
- Chronic conditions, such as overactive thyroid, diabetes
- Undergoing general anesthesia
- Lifestyle factors, such as use of stimulant drugs (including caffeine), smoking, alcohol abuse, stress (either physical or emotional)
Atrial fibrillation – Symptoms
Symptoms can vary from mild to severe. This depends on your heart function and overall health. Some people may not notice any symptoms.
Symptoms include:
- Irregular or rapid pulse or heart beat
- Racing feeling in the chest
- Palpitations, or a pounding feeling in the chest
- Dizziness, lightheadedness, or fainting
- Sweating
- Pain or pressure in the chest
- Shortness of breath
- Fatigue or weakness
- Exercise intolerance
Atrial fibrillation – Diagnosis
The doctor will:
- Ask about your symptoms and medical history
- Perform a physical exam
- Listen to your heart with a stethoscope
Tests may include:
- Blood tests
- Chest x-ray
- Electrocardiogram (EKG) — records the heart’s activity by measuring electrical currents through the heart muscle
- 24-hour holter monitor (a portable EKG that you wear as you do your daily activities)
- Echocardiogram — uses ultrasound to examine the size, shape, and motion of the heart
- Coronary angiography — allows the doctor to look for abnormalities in the arteries and evaluate the function of the heart
Atrial fibrillation – Treatment
The goals of treatment are to:
- Restore a regular rhythm, if possible.
- Keep heart rate close to normal. — Your doctor will tell you what your target heart rate is. In general, your resting rate should be between 60-80 beats per minute, and 90-115 beats per minute during moderate exercise.
- Prevent blood clots from forming.
If your doctor finds an underlying condition that is causing atrial fibrillation, this underlying condition may be treated. In some cases, heart rhythm problems return to normal without treatment.
Treatment options include:
Medication
- Drugs to slow the heart rate, such as digitalis, verapamil, diltiazem, metoprolol, atenolol
- Drugs to keep the heart in a regular rhythm, such as sotalol, propafenone, amiodarone
- Drugs to prevent clot formation, such as warfarin, dabigatran, rivaroxaban
Procedures
- Cardioversion — This is a procedure that uses an electrical current or drugs to help normalize the heart rhythm.
- Ablation — An area of the heart that is responsible for atrial fibrillation may be surgically removed or altered (ablated) with various techniques.
- Maze procedure and mini-maze procedure — The Maze procedure creates a pattern of scar tissue in the upper chambers of the heart. This makes a pathway for electrical impulses to travel through the heart and blocks the pathway for fast or irregular impulses. The Maze procedure may also be done as minimally invasive surgery (called mini-Maze ).
Lifestyle Changes
Your doctor may recommend that you make lifestyle changes, such as:
- Avoiding certain substances (eg, caffeine and other stimulants, alcohol) that may trigger another episode
- Having a regular exercise routine
If you are diagnosed with atrial fibrillation, follow your doctor’s instructions.
Atrial fibrillation – Prevention
If you have risk factors for atrial fibrillation, avoid known triggers. Also, follow your doctor’s advice for controlling chronic conditions, like heart disease and high blood pressure.