Ventricular fibrillation
Ventricular fibrillation – Definition
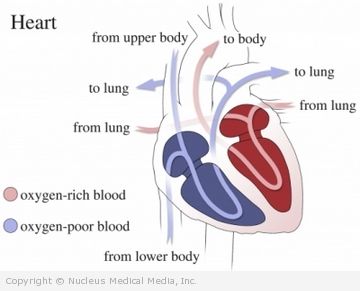
The ventricles are the large lower chamber of the heart. They are responsible for moving blood to the organs and tissues of the body. In ventricular fibrillation, the heart’s ventricles contract in a rapid and chaotic manner. As a result, little or no blood is pumped from the heart. Unless medical help is provided immediately, ventricular fibrillation will lead to cardiovascular collapse and sudden death.
Ventricular fibrillation – Causes
Causes of ventricular fibrillation include:
- Inadequate blood flow to the heart due to coronary artery disease (CAD)
- Scar tissue within the heart due to previous injury to heart, such as a heart attack (myocardial infarction)
- Congestive heart failure (CHF)
- Infection of the heart muscle ( myocarditis)
- Shock
- Electrical shock
- Drowning
- Dangerously low body temperature ( hypothermia)
- Electrolyte imbalance (eg, very low levels of potassium or magnesium in the blood)
- Drugs that affect the electrical currents of the heart (eg, sodium or potassium channel blockers)
- Low atmospheric oxygen
Ventricular fibrillation – Risk Factors
Ventricular fibrillation is most commonly associated with CAD. Factors that can increase risk of CAD will also increase the risk of ventricular fibrillation.
The following factors increase your chance of developing ventricular fibrillation. If you have any of these risk factors, tell your doctor:
- CAD
- CHF
- Heart rhythm disorder (ie, arrhythmia), especially multiple premature ventricular beats
- Previous heart attack
- Previous ventricular fibrillation
- High blood pressure
- Diabetes
- Smoking
- Excessive use of alcohol
- Drug abuse
- Stress
- High cholesterol (dyslipidemia)
- Obesity
- A high-fat diet
- A family history of cardiovascular disease
- Advancing age
Ventricular fibrillation – Symptoms
Ventricular fibrillation happens without warning. When it occurs, symptoms may include:
- Loss of consciousness within seconds
- Sudden collapse
- Seizures
- Loss of color in the skin
- Dilated pupils
- No detectable pulse, heartbeat, or blood pressure
Ventricular fibrillation – Diagnosis
Ventricular fibrillation is suspected when a person collapses suddenly and has no detectable pulse or heartbeat. The diagnosis is confirmed by electrocardiography (ECG). ECG records the heart’s activity by measuring electrical currents through the heart muscle.
Ventricular fibrillation – Treatment
Ventricular fibrillation must be treated as an extreme emergency and treatment must be administered within 4-6 minutes.
Cardiopulmonary Resuscitation (CPR)
CPR, which begins with giving chest compressions, is a temporary procedure that can help maintain some blood flow to the brain, heart, and other vital organs until trained medical personnel are available to provide more advanced treatment.
Defibrillation
In defibrillation, an electronic device is used to give an electric shock to the heart. The electric shock helps to re-establish the normal contraction rhythms of the heart. An automated external defibrillator (AED) is a portable defibrillation device. Most ambulances carry AEDs. They are also frequently found in many public places, such as sports complexes.
Defibrillation should be done as soon as equipment is available.
Anti-arrhythmic Drugs
Anti-arrhythmic drugs, such as amiodarone, lidocaine, and procainamide, may be given intravenously with continued resuscitation attempts when a person continues to fibrillate.
If the heart’s rhythm is stabilized by defibrillation, anti-arrhythmic drugs can be given to maintain the heart’s rhythm.
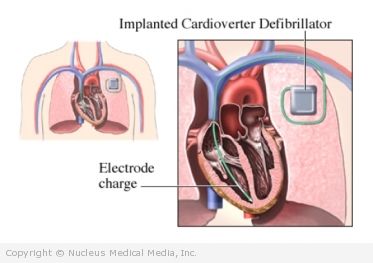
Implantable Cardioverter Defibrillator
An implantable cardioverter defibrillator (ICD) can be surgically placed in the chest to help prevent ventricular fibrillation. An ICD continuously monitors the heart’s rhythm. If it detects an abnormal beat, it automatically sends electrical impulses to restore the heart’s normal rhythm.
If you are diagnosed with ventricular fibrillation, follow your doctor’s instructions.
Ventricular fibrillation – Prevention
To help reduce your chance of getting ventricular fibrillation, take the following steps:
- Lower your risk of CAD:
- Eat a healthful diet, one that is low in saturated fat and rich in whole grains, fruits, and vegetables.
- Exercise regularly.
- If you are overweight, lose weight.
- Don’t smoke. If you smoke, quit.
- Avoid or limit your intake of caffeine, alcohol, and other substances that may contribute to arrhythmias or heart disease.
- Avoid unnecessary stress, and try to manage or control stressful situations that cannot be avoided.
- If you have a family history of this condition, see your doctor. He can evaluate your risk.
If a person is at high risk of ventricular fibrillation, an implantable cardioverter defibrillator (ICD) can be surgically placed in the chest to help stop ventricular fibrillation. In addition, anti-arrhythmic drugs may be given to try to prevent a future episode.